Bovine Tuberculosis
What is TB?
Tuberculosis (TB) is a serious bacterial disease caused by Mycobacterium, a group of bacteria that usually affects the respiratory system. Animals infected with TB may not show signs for years, but animals that appear healthy may still be capable of transmitting infection to other animals.
Tuberculosis is classified into three types:
- Human, most often caused by M. tuberculosis
- Avian, caused by M. avium
- Bovine, caused by M. bovis
Human TB, or M. tuberculosis, is rarely transmitted to animals, although it is often the type of TB that affects elephants. Avian TB is typically restricted to birds, but occasionally pigs and other animals can become affected. Bovine TB is a chronic disease that has affected animal health throughout recorded history and is capable of infecting most mammals.
More information on the disease and testing of live animals can be found in the Resources links.
California is "Accredited Free" for Bovine Tuberculosis
The U.S. Department of Agriculture (USDA) maintains a monitoring system that classifies states based on the presence of bovine TB within a state's cattle population. States, or zones within states, are classified in five categories: Accredited Free, Modified Accredited Advanced, Modified Accredited, Accreditation Preparatory and Non-Accredited. The categories are based on the number of cases of bovine TB that have been identified through surveillance programs. A state’s status can be downgraded if new cases of bovine TB are identified.
- California has been involved in bovine TB eradication programs since 1917. In 1998, the California Department of Food and Agriculture (CDFA) implemented an aggressive TB action plan with a special focus on the state’s large dairy industry.
- California achieved Accredited Free status in 1999; however, infection was detected in three Central Valley dairy herds in 2002, causing a downgrade in TB-status in April 2003. After depopulating the infected herds, extensive tracing and testing over 700,000 cattle in Tulare, Kings and Fresno counties associated with the herds, California regained its Accredited Free status in April 2005.
- In December 2007, Bovine TB was detected during routine slaughter surveillance in a Fresno County dairy cow. In May 2008, two associated Fresno County dairy herds were also confirmed to be affected by TB. On September 18, 2008, the USDA downgraded California's bovine TB status from Accredited Free to Modified Accredited Advanced. A fourth affected herd was confirmed in a San Bernardino County dairy herd in January 2009. Between these four herds, eight TB-infected cows were detected and three different genetic strain-types were isolated, suggesting these cases had three separate sources. The strains were not related to the herds detected in California in 2002-2003. Trace investigations of these herds led to about 310 separate herd tests of more than 419,000 cattle in 254 herds. Two of the affected herds (for a total of 1,500 cattle) were depopulated, while the other two herds began a "test and removal plan".
- California was on the way to regaining "TB-Free" status when, in April 2011, bovine TB was detected in a San Bernardino County dairy herd. On October 7, 2011 a second dairy herd was detected. Both herd detections followed the diagnosis of TB in a cow during routine slaughter surveillance. The different genetic strain-type of bovine TB between these two herds indicated the infections were not related. One herd went on a "test and removal plan", and the other was depopulated. On December 7, 2011 a third dairy herd in San Bernardino County, tested because it had contact with the affected herd detected October 7, 2011, was diagnosed with bovine TB. Herd TB testing revealed one animal that had suspicious lesions during necropsy; samples were confirmed positive for Mycobacterium tuberculosis complex species. The herd went on a "test and removal plan" to eradicate infection.
- On February 6, 2013 bovine TB was detected in a dairy herd in Tulare County. The diagnosis was made during trace investigation testing after a suspicious mass in a cow identified during routine slaughter inspection was confirmed positive. This herd went on a "test and removal plan".
- After the release of the affected Tulare county dairy herd from quarantine in July 2014, California was on its 24-month countdown to reapply for "TB-Free" status. Following review of the state's TB program by a USDA lead team, California achieved Accredited Free status as of August 8, 2016.
Please see our California Bovine TB Update for information on the latest bovine TB investigations and a summary table of the affected herds.
Contact your local CDFA Animal Health Branch District Office if you have any questions.
The Significance of Bovine TB
The Department is concerned about the effects of TB on the industry for several reasons. First, there is a zoonotic risk for individuals consuming raw milk and raw milk products from TB-infected animals. Second, infection with bovine TB compromises the health and reduces production in affected cattle; the presence of bovine TB can also result in trade restrictions. Additionally, there is concern about the establishment of infection in a wide host range including free-ranging wild species. While the risk of humans contracting bovine TB is extremely low, positive cases in the state’s cattle herd can negatively affect consumer confidence in milk and beef products. It is important for consumers and public health officials to understand that the TB bacteria is killed when meat is cooked and milk is pasteurized, steps that provide a final barrier to protect public health.
CDFA's objectives for the bovine tuberculosis program are to:
- Minimize the risks to public health.
- Work in partnership with United States Department of Agriculture and industry to fully recognize their roles and responsibilities in disease control and prevention.
- Use sound independent science to guide disease surveillance and control strategies.
California TB Eradication Program History
In the early 1900's, the TB eradication program began in the U.S. due to the impact of bovine TB on human and animal health. Initially, the TB program consisted of area testing, in which approximately 15% of a state's cattle population was tested each year; all herds in the state were tested every six years. This method was the primary tool used in the eradication effort until national prevalence levels of TB were greatly reduced. In 1994, California discontinued this approach because the prevalence of TB had reached such low levels that area testing was no longer an efficient method to detect the disease.
The primary method of tuberculosis surveillance shifted to slaughterhouse inspection - every bovine processed in California is examined for signs of disease. Any animals with lesions suspicious for TB are not used for human consumption, and undergo further diagnostic testing. If an infected animal is detected, an investigation is initiated by the California Department of Food and Agriculture to determine the origin location of the animal.
TB and Public Health
Bovine tuberculosis is a zoonotic disease, meaning humans can be infected by exposure to infected animals or animal products. As the prevalence of bovine TB has decreased and pasteurization has become routine, fewer human infections are traced to drinking milk. However, humans can still become infected by drinking raw milk or eating unpasteurized cheese from TB-infected animals.
Bovine tuberculosis does not threaten the quality and safety of milk and meat products produced in California. Almost all milk sold in California is pasteurized, which destroys organisms that can be harmful to humans, including tuberculosis organisms. The state’s raw milk dairies are regularly tested for tuberculosis. All cattle processed for meat are inspected for bovine TB and rejected for consumption if they show signs of the disease.
A few cases of airborne infection continue to occur among meat industry and slaughterhouse workers in regions where infection remains prevalent, including Mexico. Additionally, humans have the potential to transmit bovine tuberculosis back to cattle; however, unlike M. tuberculosis, it is rare that M. bovis is spread human to human.
- Center for Food Security and Public Health – Zoonoses
- Center for Disease Control and Prevention – Bovine Tuberculosis
- California Department of Public Health – Tuberculosis Health Information
- World Health Organization: Zoonotic Tuberculosis
Bovine TB Disease Information
Transmission
Bovine TB is most commonly spread between cattle through respiration. Invisible droplets containing TB bacteria may be exhaled or coughed out by infected animals and then inhaled by another animal. Ingestion is another route of transmission, as affected cattle shed M. bovis in milk, and may be important for infection in calves. Contaminated feed, water or the environment are less likely modes of transmission. White-tail deer are the only wildlife reservoir identified in the U.S.
Signs of the Disease
Clinical signs consist of: cough, production loss, rough hair coat, chronic weight loss, variable appetite and fluctuating fevers. Ninety percent of animals infected with tuberculosis DO NOT develop clinical signs. Animals infected with bovine TB may not show any outward signs of illness, but may eventually exhibit weight loss and a gradual decline in general health.
Lesions
In most affected cattle, lesions (granulomas, or "tubercles") are primarily found in the lymph nodes associated with the respiratory system. Lesions can also be found in the thoracic cavity, head, and mesenteric lymph nodes, as well as in the organs (lung, spleen, liver).
Formation of the TB Tubercle
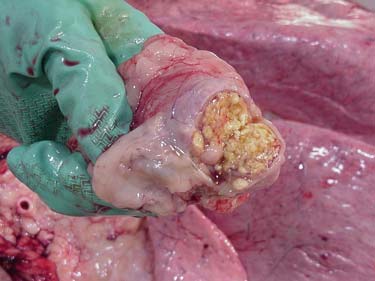
A tubercle is a granuloma consisting of inflammatory cells. When an animal’s immune system identifies M. bovis, it releases inflammatory cells, chiefly macrophages. However, M. bovis is resistant to the destructive action of the macrophage. The animal’s immune system still recognizes the TB invader and releases additional macrophages. These macrophages encapsulate the area and localized bacteria to wall it off from other tissue, and a tubercle forms. Tubercles are usually located in the respiratory lymph nodes and the lungs. The preliminary diagnosis of tuberculosis in slaughter establishments is the identification of these tubercles. Any granulomas suspected of being M. bovis granulomas are sent to an approved laboratory for further evaluation.
Resources
Contact Us
CDFA Animal Health and Food Safety Services,
Animal Health Branch
Sacramento, California 95814
Phone: 916-900-5002
Fax: 916-900-5333
Email: ahbfeedback@cdfa.ca.gov
